What Is Diabetes?
Diabetes is a long-term, serious medical condition that affects your whole body. It’s caused by a lack of insulin.
Insulin is a vital hormone produced by your pancreas that converts sugars (glucose) in your food into energy. These sugars are found in many kinds of food including bread, cereals, yoghurt, fruit, starchy vegetables, and sweets. When you eat, the sugar first goes into your bloodstream. Then your pancreas releases insulin, which is like a key that unlocks your cells and lets the sugar in so it can be converted to energy.
The three main types of diabetes happen when your body:
- Turns on itself and destroys the cells that make insulin (type 1 diabetes)
- Can’t produce enough insulin to meet your needs (type 2 diabetes)
- Becomes resistant to insulin (gestational diabetes and type 2 diabetes).
Without treatment, glucose stays in your bloodstream because it can’t get into your cells. And, even with treatment, it can be very hard to make ongoing lifestyle changes or to judge how much insulin is needed, meaning your blood glucose may go too high or too low. That can cause both short-term and long-term problems.
Importance of Good Diabetes Management
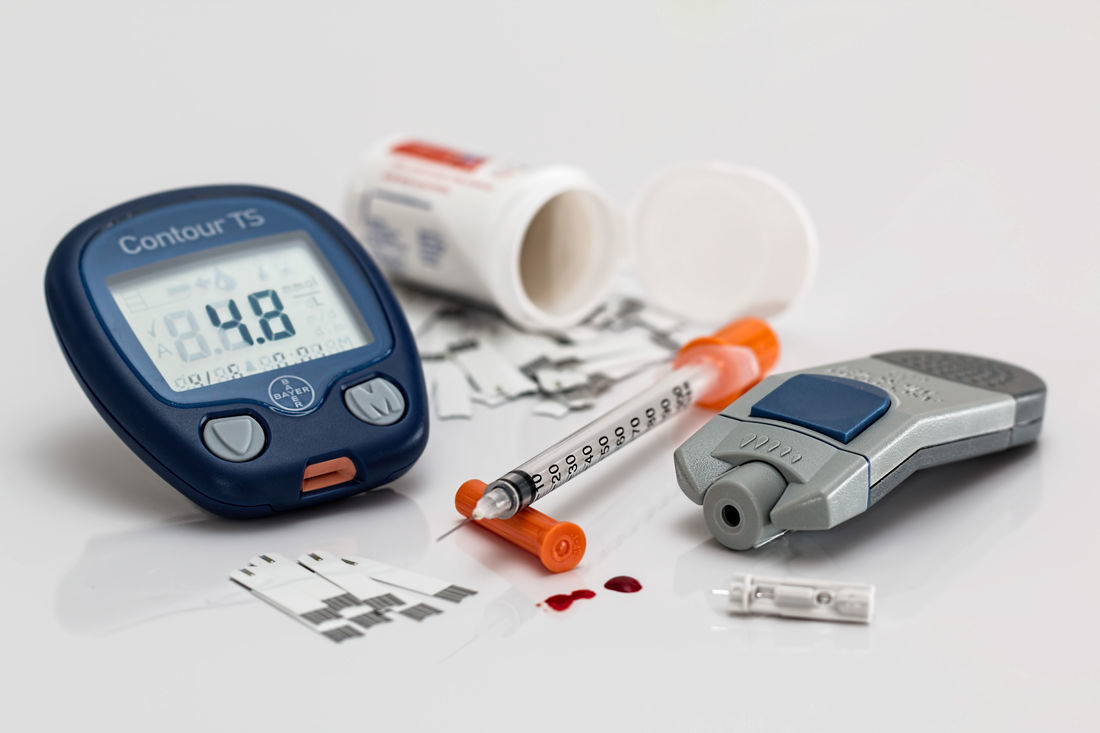
Diabetes management involves lifestyle changes and medical treatment to keep your blood sugars within normal range (or as close to it as possible). You’ll have to monitor your blood glucose regularly by pricking your fingertip and dropping the blood onto a glucose meter. You’ll also need regular screening tests to identify complications early.
Good management of diabetes is important because it’s a serious disease. People with diabetes will sometimes find that their blood sugar is too high or too low but that shouldn’t be a regular occurrence.
Complications of Diabetes
Persistently high blood sugar (hyperglycaemia) can cause blindness, kidney failure, heart disease and nerve damage. From time to time, your doctor may order an HbA1c test that measures the average amount of sugar in your blood over the last few months. If your HbA1c is too high, your doctor will probably recommend changes to your treatment and/or your lifestyle to bring it down.
Low blood sugar (hypoglycaemia), on the other hand, causes an immediate problem. Too much insulin, not enough food, or too much exercise can make your blood sugar drop below the normal level, making you feel shaky, irritable and confused. You need some fast-acting sugar quickly to fix this, which is why many people with diabetes carry jelly beans.
Managing Type 1 Diabetes
If you have type 1 diabetes, you’ll need regular insulin injections or an insulin pump because you’re not making any insulin yourself anymore. Your doctor or diabetes nurse will teach you how to inject yourself or use a pump. It’ll probably feel strange at first but, like many things, you’ll improve with practice.
Type 1 diabetes tends to strike below the age of 30. It’s usually diagnosed quite quickly because you become very unwell. Scientists are still learning about its causes but it has a strong genetic component and can’t be prevented by lifestyle changes.
However, lifestyle changes do play a significant role in managing type 1 diabetes. You’ll need to test your blood sugar regularly, eat a healthy diet, be physically active and make time for annual eye and foot checks. Your care will usually be overseen by an endocrinologist (specialist doctor).
Managing Type 2 Diabetes
About 85% of people with diabetes have type 2. There’s a genetic component to this too but modifiable lifestyle factors also play a big role. Many more of us are now overweight and inactive so type 2 diabetes is on the rise.
Type 2 diabetes often strikes in middle age and its symptoms are easily put down to ageing. Many people have had type 2 diabetes for years before it is eventually diagnosed.
You might be able to manage your type 2 diabetes by losing weight, exercising regularly, eating a healthier diet and checking your blood sugar. But it is a progressive disease and many people eventually need tablets and/or insulin alongside a healthy lifestyle. Your GP will usually provide most of your type 2 diabetes care, prescribing your tablets, arranging blood tests and drawing up a Chronic Disease Management Plan that provides Medicare funding for you to see other diabetes experts like a dietician and diabetes educator.
Managing Your Diet
You may be referred to a dietician who can help you understand how to eat well for your diabetes. Much of this advice is similar to the healthy eating advice everyone should follow. You’ll probably be advised to eat a healthy diet that encompasses the main food groups. Eating lower fat foods helps promote a healthy weight and protect your heart. Eating carbohydrates that are low on the glycaemic index (like wholegrain bread, sweet potato, milk and most fruits) helps avoid big peaks in blood sugar. And eating a healthy snack between meals can help keep your blood sugar steady throughout the day.
Self-Management of Diabetes
There are a lot of health professionals involved in diabetes care — GPs, podiatrists, optometrists, ophthalmologists, renal specialists, diabetes nurse educators and dieticians, to name just a few.
Ultimately, though, most of your diabetes care is down to you. You decide whether to have a healthy breakfast or a sugar-laden one. You decide whether to drive or walk. You decide whether to test your blood sugar or guess it.
That can feel a bit daunting but you’re not alone. Your care team are there for advice and support. They can help you learn more about diabetes management, talk through options with you and get you extra help if you need it.
On the plus side, self-management gives you a lot of choice. You can work out what kind of physical activity you like and when to fit it into your week. You decide whether you’d like treatment options based around following a set routine each day or having the most flexibility possible.
Get the Right Support to Live Well With Diabetes
It can take some time to adjust to living with diabetes. At the beginning, there’s a lot of information to take in and many things that used to be easy, like going out for dinner with friends, may now feel complicated.
If it feels overwhelming, then please talk to us. Your feelings are perfectly understandable and quite common. About 1 in 3 people with diabetes experiences anxiety, depression and distress associated with their condition. Don’t struggle alone — we can help you.
Don’t let diabetes get in the way of your dreams. There are athletes, actors, activists and adventurers who have found ways to manage their diabetes while realising their ambitions. Our skilled diabetes care team can help you handle diabetes and live your life to the max. Please make an appointment today.